However, despite extensively studied lung, kidney, and heart injury in the course of sepsis, the question of whether dysfunction of the liver is associated with mortality or a poor outcome in sepsis remains unresolved. A large body of evidence has suggested that the liver is the main target of sepsis and decompensation of liver function can trigger overwhelming inflammation, immune response, and organ damage in sepsis ( 8, 9). The liver plays a central role in homeostasis, immune surveillance, inflammation, and bacterial clearance ( 6, 7). Notably, sepsis-induced organ dysfunction is an important predictor for poor prognosis ( 3– 5). A high incidence rate and high mortality of sepsis make it one of the leading causes of death as a global health priority ( 1, 2). Sepsis is defined as a life-threatening acute organ dysfunction secondary to infection. This study may provide clinicians with some cutoff values for early intervention, which may improve the prognosis of patients with sepsis. Also, age above 65 years old, preexisting malignancy, a respiratory rate above 30 beats/min at admission, serum parameters levels within 24-h admission, containing international normalized ratio (INR) above 1.5, platelet <50 *10 ∧9/L, lactate above 4 mmol/L, and bicarbonate <22 or above 29 mmol/L are the independent risk factors for long-term mortality of patients with sepsis.Ĭonclusions: After PS matching, serum TBIL levels at more than or equal to 5 mg/dl during hospitality are associated with increased long-term mortality for patients with sepsis. Multivariate Cox hazard analysis showed that patients with TBIL at more than or equal to 5 mg/dl during sepsis exhibit 1.608 times (95% CI: 1.228–2.106) higher risk of 1-year mortality than those with TBIL levels <5 mg/dl.
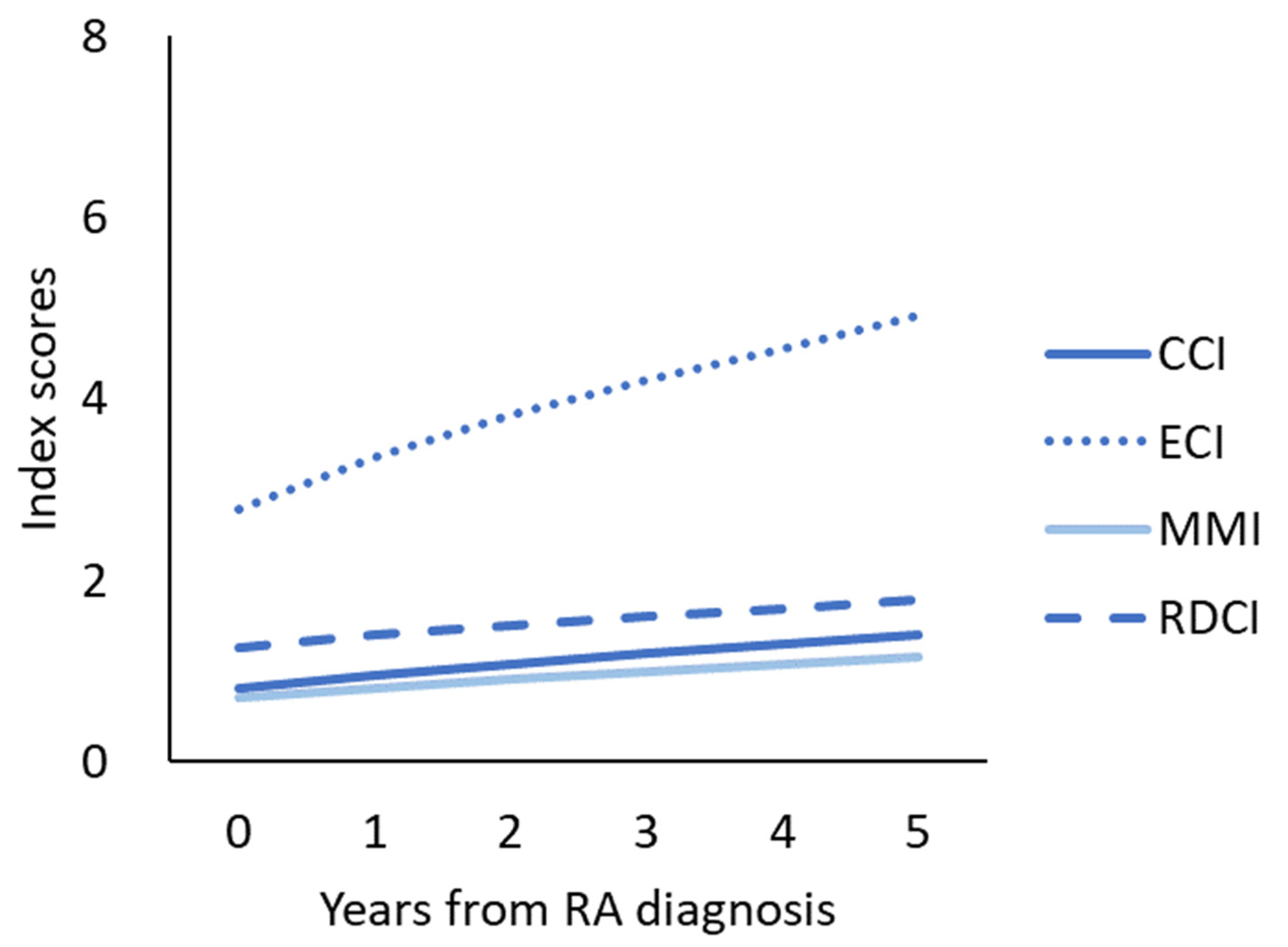
After PS matching, a survival curve demonstrated that patients with sepsis with the new onset of total bilirubin (TBIL) levels more than or equal to 5 mg/dl survived at significantly lower rates than those with TBIL levels <5 mg/dl. Results: Of 2,784 patients with sepsis, hyperbilirubinemia occurred in 544 patients (19.5%). The multivariate Cox was employed to investigate the predictors that influence a clinical outcome in sepsis. We used propensity scores (PS) to adjust the baseline differences in septic patients with hyperbilirubinemia or not. Methods: In this retrospective observational cohort study, patients with sepsis, without previous chronic liver diseases, were identified from the Medical Information Mart for the Intensive Care III MIMIC-III database. The study aims to investigate the specific stages of hyperbilirubinemia and potential risk factors on long-term outcomes in patients with sepsis.
Objective: Although hyperbilirubinemia has been associated with mortality in patients who are critically ill, yet no clinical studies dissect the effect of dynamic change of hyperbilirubinemia on long-term septic prognosis. 4Hunan Key Laboratory of Molecular Precision Medicine, Xiangya Hospital, Institute of Molecular Precision Medicine, Central South University, Changsha, China.3Department of Emergency, Xiangya Hospital, Central South University, Changsha, China.2National Clinical Research Center for Geriatric Disorders, Xiangya Hospital, Central South University, Changsha, China.1Department of Critical Care Medicine, Xiangya Hospital, Central South University, Changsha, China.Milin Peng 1,2, Fuxing Deng 1,2, Desheng Qi 2,3 * †, Zhonghua Hu 1,2,4 * † and Lina Zhang 1,2 * †
